Living with chronic stomach pain, bloating, or unpredictable bathroom habits can feel isolating. You might have been told you have Irritable Bowel Syndrome, a condition defined by functional gastrointestinal distress without visible physical damage. Or perhaps your doctor mentioned Inflammatory Bowel Disease, which involves chronic inflammation and structural damage to the digestive tract. The names sound similar, and the symptoms often overlap, but these are two very different conditions with distinct causes, risks, and treatments.
Confusing the two isn't just a matter of semantics. Mistaking IBD for IBS could mean missing signs of serious intestinal damage. On the flip side, treating IBS as if it were IBD might lead to unnecessary anxiety or aggressive medications. Let’s break down exactly what is happening in your body, how doctors tell them apart, and what your next steps should look like.
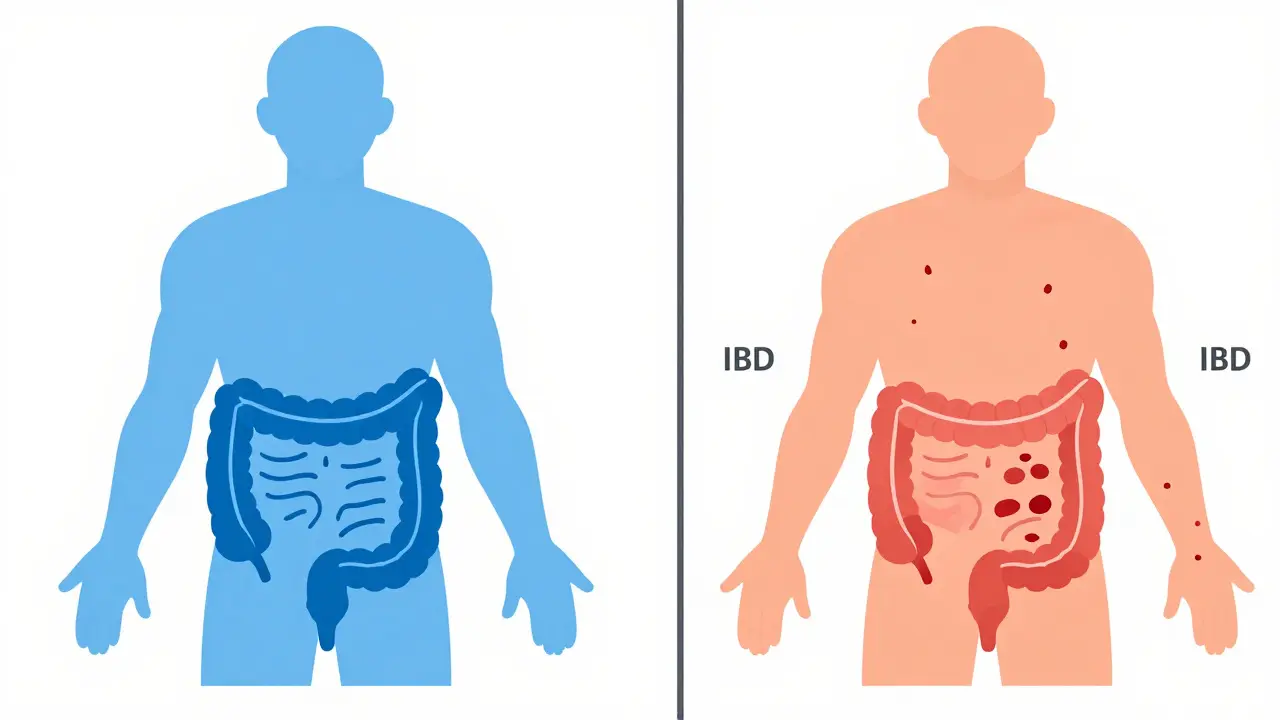
The Core Difference: Function vs. Structure
To understand why these conditions require different approaches, you need to look at what is actually happening inside your gut. The simplest way to think about it is this: IBS is a problem with how your gut works, while IBD is a problem with the structure of your gut.
Irritable Bowel Syndrome (IBS) is classified as a functional disorder. This means that if a gastroenterologist looks at your colon using a camera or takes blood samples, everything will appear normal. There is no swelling, no bleeding, and no tissue damage. However, the nerves in your gut are hypersensitive, and the muscles may contract too strongly or too weakly. It’s like having a car with a perfectly fine engine that keeps throwing error codes because the sensors are overly sensitive. According to the Rome IV criteria, established by international experts in 2016, IBS is diagnosed based on specific symptom patterns rather than physical abnormalities.
In contrast, Inflammatory Bowel Disease (IBD) is a structural disease. IBD is an umbrella term that primarily includes Crohn's disease, first described by Dr. Burrill B. Crohn in 1932 and Ulcerative colitis, documented as early as 1859. In these conditions, your immune system mistakenly attacks your own digestive tract. This causes visible inflammation, ulcers, and thickening of the intestinal walls. If a doctor performs an endoscopy on someone with active IBD, they will see redness, sores, and potentially bleeding. This structural damage is what leads to the more severe complications associated with IBD.
Symptom Checklist: What Should Raise Your Alarm?
Both conditions share common complaints like abdominal cramping, diarrhea, and bloating. This overlap is why self-diagnosis is risky. However, there are specific "alarm features" that point strongly toward IBD rather than IBS. Pay attention to these distinctions.
- Blood in the stool: This is the biggest red flag. Blood in your stool is never normal. While IBS can cause mucus in the stool (seen in about 45% of cases), it does not cause bleeding. Bloody stools are present in up to 92% of ulcerative colitis cases during flares. If you see bright red blood or black, tarry stools, seek medical attention immediately.
- Unexplained weight loss: Losing weight without trying is a sign that your body isn’t absorbing nutrients properly due to intestinal damage. About 65% of IBD patients experience this during flare-ups. IBS does not cause malabsorption or significant weight loss.
- Fever and night sweats: A low-grade fever suggests systemic inflammation. Fever occurs in about 40% of moderate-to-severe IBD cases. IBS is not an inflammatory condition, so it does not cause fever.
- Anemia: Chronic bleeding from ulcers in the gut leads to iron-deficiency anemia. This is a common complication of IBD but is not associated with IBS.
- Extraintestinal symptoms: IBD affects the whole body. Up to 30% of IBD patients develop joint pain (arthritis), and others may experience eye inflammation (uveitis) or skin rashes like erythema nodosum. IBS stays confined to the gastrointestinal tract.
If your symptoms are limited to pain, bloating, gas, and changes in bowel frequency (constipation or diarrhea) without any of the alarm features above, IBS is more likely. Studies show that IBS affects 10-15% of the global population, with women making up about 65% of those cases.

How Doctors Diagnose the Two Conditions
Because the symptoms overlap, diagnosis relies heavily on testing to rule out structural damage. The diagnostic paths for IBS and IBD are fundamentally different.
| Test Type | IBS (Functional) | IBD (Inflammatory) |
|---|---|---|
| Blood Tests | Normal results. No signs of infection or inflammation. | Elevated markers. C-reactive protein (CRP) often exceeds 5 mg/L; ferritin may be low due to anemia. |
| Stool Tests | Normal fecal calprotectin levels (<50 µg/g). No blood or parasites. | High fecal calprotectin (>250 µg/g). Presence of occult blood or white blood cells. |
| Endoscopy | Used only to rule out other causes. Colon appears visually normal. | Primary diagnostic tool. Shows redness, ulcers, and granulomas. Biopsies confirm inflammation. |
| Imaging | Rarely needed. CT scans are typically normal. | MRI enterography or CT scans used to check for strictures, fistulas, or deep tissue inflammation. |
For IBS, doctors often use a "diagnosis of exclusion." This means they test for other things first. If your blood work, stool tests, and colonoscopy come back clean, and you meet the Rome IV criteria for symptom duration (at least one day per week for three months), you are likely diagnosed with IBS.
For IBD, the diagnosis is positive. Doctors look for evidence of inflammation. Fecal calprotectin is a key marker here. It’s a protein found in neutrophils (white blood cells) that increases when there is intestinal inflammation. In 95% of IBD patients, this level is significantly elevated. In IBS patients, it remains normal. Additionally, colonoscopy with biopsy is the gold standard for IBD, allowing pathologists to see microscopic changes in the tissue that confirm Crohn's disease or ulcerative colitis.
Treatment Paths: Managing Symptoms vs. Healing Tissue
Because the underlying mechanisms differ, the treatments do not mix. Taking IBD medication for IBS is ineffective and exposes you to unnecessary side effects. Conversely, relying on diet alone for IBD can allow dangerous inflammation to progress.
Managing IBS Since IBS is a functional issue involving the brain-gut connection, treatment focuses on calming the nervous system and adjusting gut motility.
- Dietary Changes: The low-FODMAP diet is highly effective, reducing symptoms in 76% of patients according to a 2021 systematic review. This involves temporarily restricting fermentable carbohydrates that feed gut bacteria and cause gas.
- Neuromodulators: Low-dose tricyclic antidepressants or SSRIs are often prescribed. These don’t treat depression in this context; they modulate the nerve signals between your gut and brain, reducing pain perception.
- Gut-Directed Therapies: Medications like eluxadoline can help control diarrhea and pain in IBS-D (diarrhea-predominant) patients by targeting specific receptors in the intestine.
- Stress Management: Since stress exacerbates IBS symptoms, cognitive behavioral therapy (CBT) and mindfulness practices are frequently recommended.
Treating IBD IBD requires medical intervention to suppress the immune system and heal the intestinal lining.
- Anti-Inflammatories: Aminosalicylates (like mesalamine) are often the first line of defense for mild ulcerative colitis.
- Corticosteroids: Drugs like prednisone are used short-term to quickly reduce severe inflammation during flares, though they are not suitable for long-term use due to side effects.
- Biologics: These targeted therapies, such as infliximab (an anti-TNF agent) or vedolizumab, block specific proteins involved in inflammation. Infliximab achieves clinical remission in 50-60% of Crohn's patients within 14 weeks.
- Immunomodulators: Medications like azathioprine help suppress the overall immune response to prevent future flares.
It is crucial to note that while IBS does not turn into IBD, it is possible to have both simultaneously. About 22-35% of IBD patients who are in remission still meet the criteria for IBS. In these cases, doctors treat the IBD with biologics to stop the damage, and then manage the remaining IBS-like symptoms with diet and neuromodulators.

Long-Term Outlook and Complications
Understanding the prognosis helps set realistic expectations. IBS is chronic but benign. It does not cause permanent damage to your intestines, nor does it increase your risk of colorectal cancer. As the Mayo Clinic states, IBS does not develop into IBD. However, the impact on quality of life can be severe. Many IBS patients report sacrificing social activities, travel, or even sleep to manage their symptoms.
IBD, on the other hand, carries significant long-term risks if left uncontrolled. Chronic inflammation can lead to:
- Strictures: Scarring that narrows the intestine, occurring in 33% of Crohn's patients within 10 years.
- Fistulas: Abnormal tunnels connecting the intestine to other organs, affecting 17% of Crohn's patients.
- Colorectal Cancer: Patients with pancolitis (inflammation of the entire colon) face a 2% annual risk of cancer after 10 years of disease. Regular surveillance colonoscopies are essential.
- Toxic Megacolon: A rare but life-threatening complication where the colon expands rapidly, requiring emergency surgery.
Early diagnosis and consistent treatment of IBD can induce remission, allowing the mucosa to heal and significantly reducing these risks. For IBS, the goal is symptom control and improving daily functioning through lifestyle adjustments and targeted medications.
When to See a Doctor
You should not ignore persistent digestive issues. While occasional bloating or irregularity is normal, chronic symptoms warrant professional evaluation. Specifically, see a doctor right away if you experience:
- Blood in your stool (bright red or dark/tarry)
- Unintentional weight loss
- Pain that wakes you up from sleep
- Family history of colorectal cancer or IBD
- Symptoms starting after age 50
A gastroenterologist can perform the necessary tests to distinguish between functional and inflammatory causes. Getting the right diagnosis is the first step toward getting relief. Whether you are dealing with the sensitivity of IBS or the inflammation of IBD, effective management strategies exist. The key is knowing which one you have.
Can IBS turn into IBD over time?
No, IBS cannot turn into IBD. They are distinct conditions with different causes. IBS is a functional disorder with no structural damage, while IBD is an inflammatory autoimmune disease. However, it is possible to have both conditions simultaneously, which can complicate diagnosis.
What is the best test to distinguish IBS from IBD?
Fecal calprotectin is a highly effective non-invasive test. Elevated levels indicate intestinal inflammation, pointing toward IBD. Normal levels suggest IBS. However, a colonoscopy with biopsy is the gold standard for definitively diagnosing IBD and ruling out other structural issues.
Does IBS cause fatigue?
Yes, many people with IBS report fatigue, often due to poor sleep caused by nighttime symptoms or the mental burden of managing chronic discomfort. However, unlike IBD, IBS does not cause fatigue through systemic inflammation or anemia.
Are there specific foods that trigger IBD?
While no specific food causes IBD, certain foods can worsen symptoms during flares. High-fiber foods, dairy, and spicy foods are common triggers. Unlike IBS, where diet plays a central role in management, IBD treatment primarily relies on medication to control inflammation, though dietary adjustments help manage symptoms.
Is IBS considered a disability?
Severe IBS can qualify as a disability under laws like the ADA (Americans with Disabilities Act) if it substantially limits major life activities. Many employers offer accommodations for frequent bathroom breaks or flexible schedules. IBD is also recognized as a disability when it significantly impairs function.


 Medications
Medications





Brian LeClercq
May 5, 2026 AT 23:19This entire article is a classic example of medical gaslighting designed to keep you dependent on the pharmaceutical industrial complex. They want you to believe that your gut issues are either 'all in your head' (IBS) or require lifelong immunosuppression (IBD). The truth is that modern diets, specifically high-fructose corn syrup and glyphosate residues, are destroying the human microbiome. You don't need a colonoscopy; you need to stop eating processed garbage. But sure, take another pill while your body rots from the inside out.
Natali Brown
May 6, 2026 AT 02:59I completely agree with the sentiment here, though perhaps the delivery was a bit harsh! 😊 It is so true that we often overlook the environmental factors contributing to our health. I have found that keeping a detailed food diary helps identify triggers much better than any expensive test. When I started tracking my stress levels alongside my meals, I noticed a clear pattern where high-stress days led to immediate bloating, regardless of what I ate. It’s amazing how interconnected everything is, isn’t it? 🌿
Frances Kendall
May 7, 2026 AT 11:12The distinction between functional and structural damage is profound when viewed through the lens of patient experience. For those with IBS, the pain is real, yet invisible, which often leads to a sense of isolation and invalidation by healthcare providers who cannot see the pathology. This epistemological gap creates a unique psychological burden. Conversely, IBD patients face the tangible reality of tissue destruction, which commands immediate medical attention but carries its own stigma regarding hygiene and bodily function. Both groups suffer from a lack of societal understanding, albeit in different forms.
swetha r
May 8, 2026 AT 19:13Why does no one talk about the electromagnetic fields from our phones causing this inflammation? I read somewhere that 5G disrupts the cellular integrity of the gut lining. It’s all connected. The doctors are paid off by big tech to ignore the real cause. I stopped using my phone near my bed and my bloating went away. Coincidence? I think not. Wake up sheeple. 👁️
Kelsey Thomas
May 10, 2026 AT 01:02Hey everyone! 👋 Just wanted to add that low-FODMAP is great, but please remember to reintroduce foods slowly. Don’t stay on the restriction phase forever! Your gut needs diversity to thrive. Also, hydration is key! 💧✨
Derick Garcia
May 10, 2026 AT 02:26It is intellectually dishonest to conflate these two distinct pathologies under the guise of 'similar symptoms.' The etiology of Irritable Bowel Syndrome remains idiopathic and multifactorial, involving visceral hypersensitivity and altered motility, whereas Inflammatory Bowel Disease is unequivocally an autoimmune-mediated inflammatory process. To suggest that dietary changes alone can mitigate the structural damage caused by Crohn's disease or Ulcerative Colitis is not only medically inaccurate but dangerously negligent. One must respect the scientific rigor required to differentiate between a functional disorder and an organic disease.
Abhimanyu Pandey
May 11, 2026 AT 16:34They want you to think it’s just 'stress' or 'diet';; but look at the data;; the incidence rates are skyrocketing;; why?; Because they are poisoning the water supply;; fluoride;; chlorine;; heavy metals;; it’s a systematic dismantling of the human immune system;; and they profit from selling you pills to fix what they broke;; do not trust them;; they are watching you;; every symptom is a message;; decode it;; before it’s too late;;